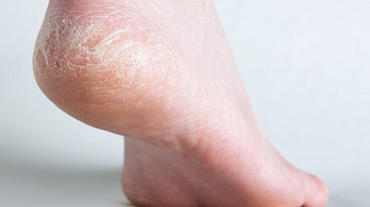
The foot complications arising from diabetes are serious and often difficult to treat and may predispose people to further complications. When it comes to diabetes and feet, prevention is the goal.
If diabetes is poorly controlled for a long period of time, this may lead to:
- Nerve damage, or ‘peripheral neuropathy’, which impairs sensation to the feet, and/or
- Reduced blood supply, also know as ‘poor circulation’.
Nerve damage may mean a person loses full sensation in the feet. If a person has poor circulation, any injuries or infections to the feet (i.e. cuts, burns, or scratches) will take longer to heal. This is due to less blood flowing into the arteries in the feet. Blood provides energy to working muscles and aids in healing any tissue damage.
People with poor circulation need to take extra care to protect their feet from injury.
Most foot problems in people with diabetes occur when injuries – and often infections – go unnoticed and untreated, or when healing is delayed due to poor circulation.
To prevent problems:
- Protect your feet from injury
- Inspect your feet every day (your podiatrist can show you how)
- See your podiatrist immediately if a cut or wound is not healing
National Diabetes Health Care Guidelines recommend people with diabetes have their feet checked by a podiatrist at least every 12 months.